Ensure all treatments receive authorization Copied
Practices can now prevent treatments being marked as not needing insurance authorization in the Ins. Auth/Fin. Counseling queue. This ensures all treatments receive insurance authorization, which is especially important for patients with a change in insurance that may require authorization for a treatment before it is covered.
To remove this option from the Ins. Auth/Fin. Counseling queue:
-
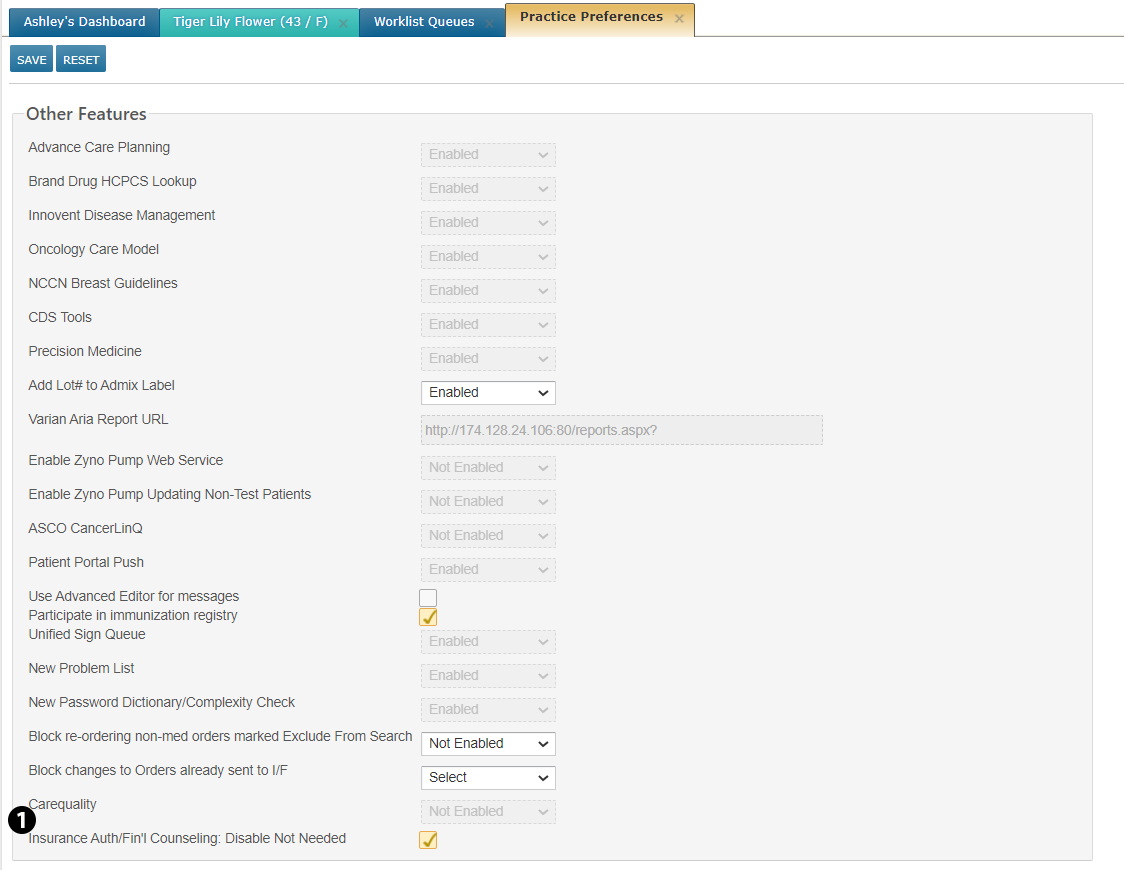
Go to ADMIN > Practice Preferences.
-
Under Other Features, turn on the new Ins. Auth/Fin. Counseling: Disable Not Needed option (see callout 1).
-
SAVE your changes.
-
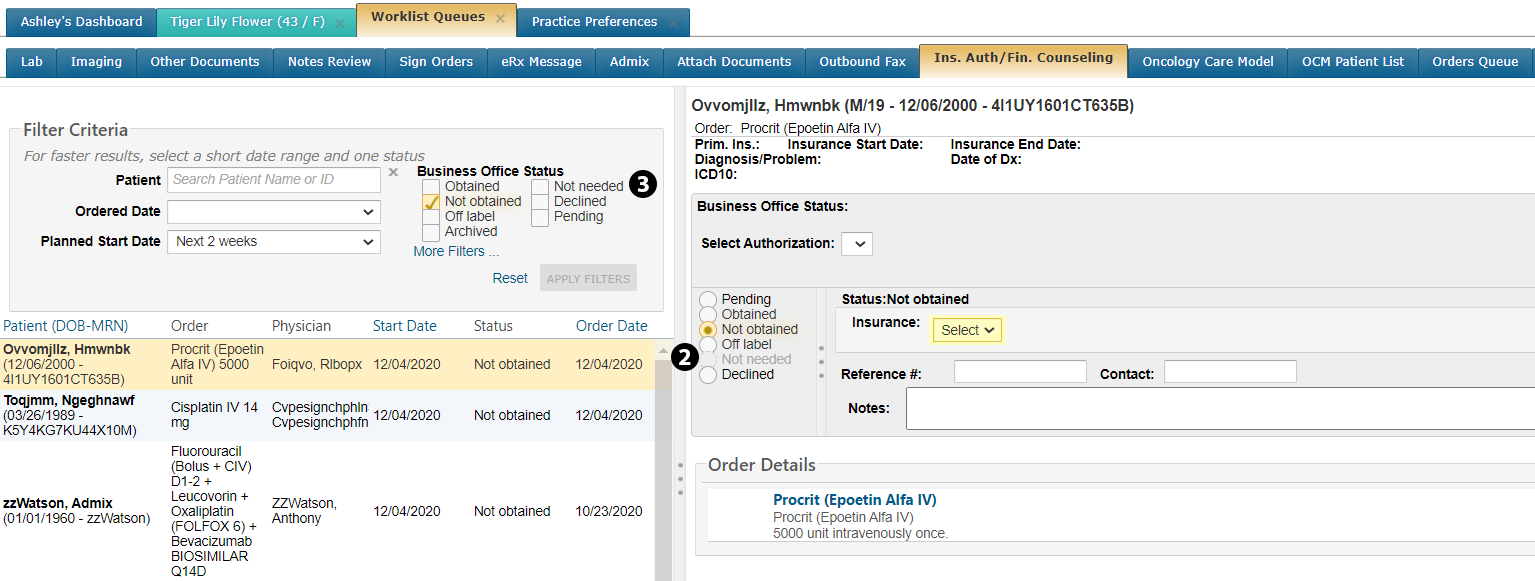
Now when working in the Ins. Auth/Fin. Counseling queue, the Not needed option will be unavailable for selection going forward (see callout 2).
-
You will still be able to choose the Not needed option in the Filter Criteria (see callout 3) to see prior treatments that were marked as not needing authorization.