Depression Status: Corrected terminology for declined assessments Copied
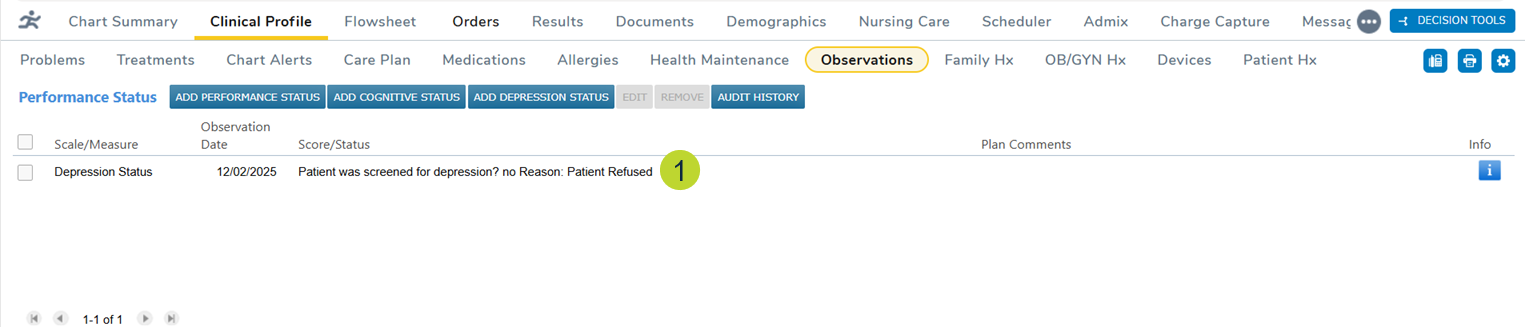
When a patient declines to complete a depression assessment, the Observations tab will correctly display “Patient Refused” instead of “Patient declined treatment” (callout 1).
What’s changing
Previously, selecting “Patient declined to complete assessment” under Clinical Profile > Patient Hx > Depression Screening & Plan incorrectly displayed as “Patient declined treatment” in the Observations tab.
This created confusion by suggesting the screening was positive, but treatment was refused, rather than indicating the assessment itself wasn’t completed.
The terminology now accurately reflects that the patient declined the screening, not the treatment.
Why this matters
Accurate depression screening documentation supports CMS requirements and prevents misinterpretation of patient refusal status in the clinical record.
